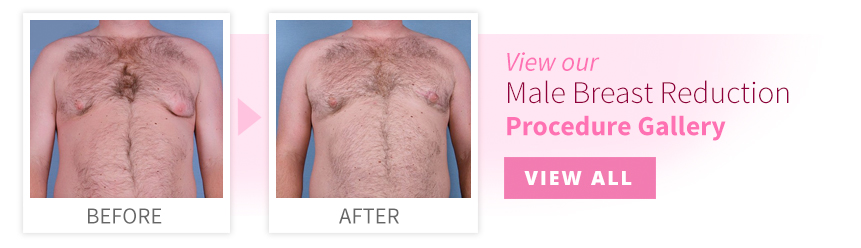
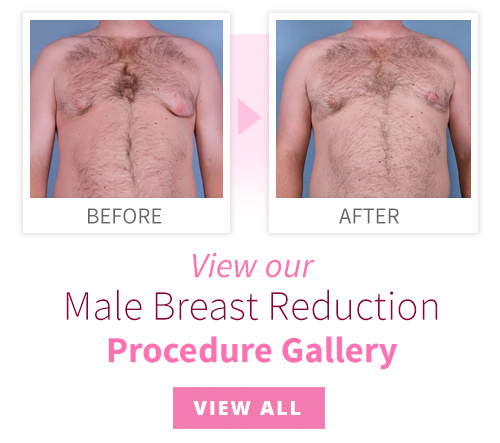
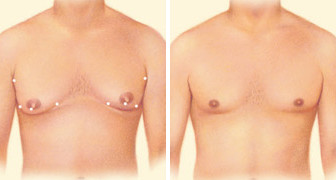
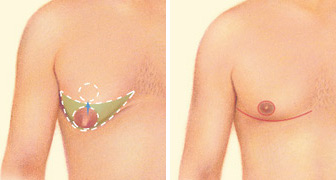
Gynecomastia (enlarged male breasts) although rarely discussed, is a common condition. Gynecomastia affects approximately 40 to 60 percent of men. There is no known cause for gynecomastia, although there has been some correlation with various drugs or medical conditions.
Men who feel self-conscious about their appearance are helped with breast-reduction surgery. This procedure involves the removal of fat and/or glandular tissue from the breasts and in extreme cases may even involve removal of excess skin. This results in a more contoured chest that is flatter and firmer.
Procedure Details: Breast Reduction
Procedure: Reduce the size of overly large, pendulous breasts by removing excess skin and tissue and repositioning remaining tissue and nipples.
Length: 3 to 4 hours.
Anesthesia: Local with sedation, or general.
In/Outpatient: Usually outpatient. Sometimes inpatient.
Side Effects: Temporary Swelling, bruising, edema, transient altered nipple, and numbness. Permanent scars.
Recovery: You may shower the following day and get back to non-strenuous work activity within a week; exercise after 3-5 weeks.
Duration of Results: Variable; gravity, aging, and weight changes may cause eventual sagging, but significantly less than without a breast reduction.
Questions & Answers
What is gynecomastia surgery?
Gynecomastia surgery reduces breast size, flattening and enhancing the chest contours.
In severe cases of gynecomastia, the weight of excess breast tissue may cause the breasts to sag and stretch the areola (the dark skin surrounding the nipple). In these cases the position and size of the areola can be surgically improved and excess skin may be reduced.
Plastic surgery to correct gynecomastia is technically called reduction mammaplasty.
What is gynecomastia?
Gynecomastia is a condition of over-developed or enlarged breasts in men that can occur at any age. The condition can be the result of hormonal changes, heredity, obesity, or the use of certain drugs.
Gynecomastia can cause emotional discomfort and impair your self confidence. Some men may even avoid certain physical activities and intimacy simply to hide their condition.
Gynecomastia is characterized by:
- Excess localized fat
- Excess glandular tissue development
- Sometimes excess breast skin
- Presence unilaterally (one breast) or bilaterally (both breasts)
Gynecomastia surgery cost
Your cost will be based on your individual plan and procedure.
Call us at (352) 629-8154 to set up a FREE Consultation.
We offer patient financing plans, so be sure to ask.
Gynecomastia surgery costs may include:
- Anesthesia fees
- Hospital or surgical facility costs
- Medical tests
- Post-surgery garments
- Prescriptions for medication
- Surgeon’s fee
Your satisfaction involves more than a fee. When choosing a board-certified plastic surgeon for gynecomastia surgery, remember that the surgeon’s experience and your comfort with him or her are just as important as the final cost of the surgery.
Gynecomastia surgery and health insurance coverage
In most cases, correction of gynecomastia is not eligible for insurance coverage. However, each insurance policy varies greatly. Carefully review your policy to determine coverage.
The American Society of Plastic Surgeons has published a position paper for physicians and insurers defining the recommended criteria for reconstructive cases of gynecomastia. Ask your physician for a copy of this document to submit to your insurer.
Gynecomastia surgery candidates
Gynecomastia surgery candidates include:
- Men whose condition cannot be corrected through alternative medical treatments
- Healthy individuals who do not have a life-threatening illness or medical conditions that can impair healing
- Non-smokers and non-drug users
- Men with a positive outlook and specific goals in mind for improving the physical symptoms of gynecomastia
- Men who are physically healthy and of relatively normal weight
- Men who have realistic expectations
- Men whose breast development has stabilized
- Men who are bothered by the feeling that their breasts are too large
Adolescents may benefit from surgery, although secondary procedures may be needed in the future should breast development continue.
Gynecomastia surgery recovery
During your gynecomastia surgery recovery period, dressings or bandages will be applied to your incisions and an elastic bandage or support garment may be used to minimize swelling and support your new chest contour as it heals after surgery.
A small, thin tube may be temporarily placed under the skin to drain any excess blood or fluid that may collect.
You will be given specific instructions that may include how to care for the surgical site and drains, medications to apply or take orally to aid healing and reduce the potential for infection, specific concerns to look for at the surgical site or in your general health, and when to follow up with your plastic surgeon.
Be sure to ask your plastic surgeon specific questions about what you can expect during your individual recovery period.
- Where will I be taken after my surgery is complete?
- What medication will I be given or prescribed after surgery?
- Will I have dressings/bandages after surgery? When will they be removed?
- Are stitches removed? When?
- When can I resume normal activity and exercise?
- When do I return for follow-up care?
It’s very important to follow your plastic surgeon’s instructions and attend follow-up visits as scheduled.
The final results of gynecomastia surgery are permanent in many cases. However, if gynecomastia resulted from the use of certain prescription medications, drugs (including steroids), or weight gain you must be fully free from these substances and remain at a stable weight in order to maintain your results.
Please discuss this with your physician before making changes to your prescription medications.
Recovering from gynecomastia surgery at home
If you experience shortness of breath, chest pains, or unusual heart beats, seek medical attention immediately. Should any of these complications occur, you may require hospitalization and additional treatment.
Following your physician’s instructions is essential to the success of your surgery.
It’s important that the surgical incisions are not subjected to excessive force, swelling, abrasion, or motion during the time of healing. Your doctor will give you specific instructions on how to care for yourself.
Gynecomastia surgery before and after results
Gynecomastia surgery results are immediately visible. Over time, post-surgical swelling will resolve and incision lines will fade. Satisfaction with your new image should continue to grow as you recover from surgery.
The final results of your gynecomastia surgery will appear over the next few months. Incision lines are permanent, but will continue to fade over time.
You can view gynecomastia surgery before and after photos in our online gallery.
Gynecomastia surgery scars
Any surgical treatment to correct gynecomastia will require incisions. While most incision lines are concealed within natural contours, some may be visible and are a necessary result of male breast reduction surgery.
All gynecomastia surgery scars are permanent, even though some scars may be concealed in the natural contours of the breast. Your improved upper body will likely enhance your self-image and confidence, whether in a shirt and tie, a t-shirt, or baring your chest at the beach.
The practices of medicine/surgery is not an exact science. Although good results are expected from your procedure, there is no guarantee. In some situations, it may not be possible to achieve optimal results with a single surgical procedure to treat gynecomastia.
Another surgery may be necessary:
- To perform additional tightening or repositioning of the breasts
- To treat any complications that may occur
Gynecomastia surgery procedure steps
A gynecomastia procedure includes the following steps:
Anesthesia
Medications are administered for your comfort during the surgical procedures. The options include intravenous sedation and general anesthesia. Your doctor will recommend the best option for you.
Liposuction technique
In cases where gynecomastia is primarily the result of excess fatty tissue, liposuction techniques alone may be used. This requires insertion of a cannula, a thin hollow tube, through several small incisions.
The cannula is moved back and forth in a controlled motion to loosen the excess fat, which is then removed from the body by vacuum suction.
There are various liposuction techniques that may be used; the technique most appropriate in your case will be defined prior to your procedure.
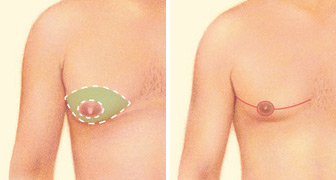
Excision technique
Excision techniques are recommended where glandular breast tissue or excess skin must be removed to correct gynecomastia. Excision also is necessary if the areola will be reduced or the nipple will be repositioned to a more natural male contour. Incision patterns vary depending on the specific conditions and surgical preference.
Combination of liposuction & excision techniques
Sometimes gynecomastia is treated with both liposuction and excision.
Gynecomastia surgery risks and safety
The decision to have plastic surgery is extremely personal, and you will have to decide if the benefits will achieve your goals and if the risks and potential complications of gynecomastia surgery are acceptable.
You will be asked to sign consent forms to ensure that you fully understand the procedure and any risks and potential complications.
Gynecomastia surgery risks include:
- Reactions to tape, suture materials, glues, topical preparations or injected agents
- Anesthesia risks
- Bleeding (hematoma)
- Blood clots
- Breast asymmetry
- Breast contour and shape irregularities
- Changes in nipple or breast sensation may be temporary or permanent
- Damage to deeper structures – such as nerves, blood vessels, muscles, and lungs – can occur and may be temporary or permanent
- Deep vein thrombosis, cardiac and pulmonary complications
- Fatty tissue found in the breast might die (fat necrosis)
- Fluid accumulation (seroma)
- Infection
- Persistent pain
- Poor wound healing
- Possibility of revisional surgery
- Unfavorable scarring
These risks and others will be fully discussed prior to your consent. It’s important that you address all your questions directly with your plastic surgeon.
Your gynecomastia surgery consultation
During your gynecomastia surgery consultation be prepared to discuss:
- Your surgical goals
- Medical conditions, drug allergies and medical treatments
- Current medications, vitamins, herbal supplements, alcohol, tobacco and recreational drug use (including steroids)
- Previous surgeries
Your gynecomastia surgeon may also:
- Evaluate your general health status and any pre-existing health conditions or risk factors
- Perform diagnostic testing to determine the underlying cause of gynecomastia; this may include testing of your endocrine function
- Examine your breasts and may take detailed measurements of their size and shape, skin quality, and placement of your nipples and areolas
- Take photographs for your medical records
- Discuss your options
- Recommend a course of treatment
- Discuss likely outcomes of gynecomastia correction and any risks or potential complications
- Discuss the use of anesthesia during your procedure
Be sure to ask questions. To help, we have prepared a checklist of questions to ask your gynecomastia surgeon that you can take with you to your consultation. (see tab titled “Questions to ask your gynecomastia surgeon”).
It’s very important to understand all aspects of your surgical prcoedure. It’s natural to feel some anxiety, whether it’s excitement for your anticipated new look or a bit of preoperative stress. Don’t be shy about discussing these feelings with your plastic surgeon.
Preparing for gynecomastia surgery
In preparing for gynecomastia surgery, you may be asked to:
- Get lab testing or a medical evaluation
- Take certain medications or adjust your current medications
- Stop smoking
- Avoid taking aspirin, anti-inflammatory drugs and herbal supplements as they can increase bleeding
The success and safety of your gynecomastia procedure depends very much on your complete candidness during your consultation. You’ll be asked a number of questions about your health, desires, and lifestyle.
Male breast reduction surgery may be performed in an accredited, office-based surgical facility, licensed ambulatory surgical center, or a hospital. Be sure to arrange for someone to drive you to and from surgery and to stay with you for at least the first night following surgery.
Gynecomastia words to know
- Areola: Pigmented skin surrounding the nipple.
- Bilateral gynecomastia: A condition of over-developed or enlarged breasts in men affecting both breasts.
- Endocrine system: A group of glands that make hormones which help to control activities in your body such as reproduction, metabolism, growth and development. Testing of your endocrine system may be done to look for signs of diabetes, thyroid disorders, growth hormone deficiency, osteoporosis, hypertension and obesity.
- Excision: To remove the skin.
- General anesthesia: Drugs and/or gases used during an operation to relieve pain and alter consciousness.
- Hematoma: Blood pooling beneath the skin.
- Intravenous sedation: Sedatives administered by injection into a vein to help you relax.
- Liposuction: Also called lipoplasty or suction lipectomy, this procedure vacuums out fat from beneath the skin’s surface to reduce fullness.
- Local anesthesia: A drug injected directly to the site of an incision during an operation to relieve pain.
- Reduction mammaplasty: The surgical removal of breast tissue to reduce the size of breasts.
- Sutures: Stitches used by surgeons to hold skin and tissue together.
- Unilateral gynecomastia: A condition of over-developed or enlarged breasts in men affecting just one breast.
Questions to ask your gynecomastia surgeon
Use this checklist as a guide during your gynecomastia surgery consultation:
- Are you certified by the American Board of Plastic Surgery?
- Were you trained specifically in the field of plastic surgery?
- How many years of plastic surgery training have you had?
- Do you have hospital privileges to perform this procedure? If so, at which hospitals?
- Is the office-based surgical facility accredited by a nationally- or state-recognized accrediting agency, or is it state-licensed or Medicare-certified?
- Am I a good candidate for this procedure?
- What will be expected of me to get the best results?
- Where and how will you perform my procedure?
- What surgical technique is recommended for me?
- How long of a recovery period can I expect, and what kind of help will I need during my recovery?
- What are the risks and complications associated with my procedure?
- How are complications handled?
- What are my options if I am dissatisfied with the outcome of my surgery?
- Do you have before-and-after photos I can look at for this procedure and what results are reasonable for me?
Choose a gynecomastia surgeon you can trust
Gynecomastia surgery involves many choices. The first and most important is selecting a member of the American Society of Plastic Surgeons (ASPS) surgeon you can trust.
- ASPS member surgeons meet rigorous standards:
- Board certification by the American Board of Plastic Surgery® (ABPS) or in Canada by The Royal College of Physicians and Surgeons of Canada®
- Complete at least six years of surgical training following medical school with a minimum of three years of plastic surgery residency training
- Pass comprehensive oral and written exams
- Graduate from an accredited medical school
- Complete continuing medical education, including patient safety, each year
- Perform surgery in accredited, state-licensed, or Medicare-certified surgical facilities
Do not be confused by other official sounding boards and certifications.
The ABPS is recognized by the American Board of Medical Specialties (ABMS), which has approved medical specialty boards since 1934. There is no ABMS recognized certifying board with “cosmetic surgery” in its name.
By choosing a member of the American Society of Plastic Surgeons, you can be assured that you are choosing a qualified, highly trained plastic surgeon who is board-certified by the ABPS or The Royal College of Physicians and Surgeons of Canada.
Q&A Content Copyright © American Society of Plastic Surgeons